Decreasing end-of-life disparities of a doubly vulnerable population
Facing Alzheimer’s disease in a loved one is challenging under any circumstances but may be even more challenging when the patient is lesbian, gay, bisexual, or transgender (LGBT).
Regenstrief Institute Research Scientist and Indiana University School of Medicine faculty member Alexia Torke, M.D., M.S., has received a grant from the National Institutes of Health (NIH) to gain insight into the needs and experiences of this doubly vulnerable population – LGBT older adults with Alzheimer’s disease – and their surrogate decision makers.
“With this study we are taking a step on the path towards decreasing health disparities among the LGBT community in the context of end-of-life care,” said Dr. Torke. “We need to know more about their needs and experiences so we can develop tools and resources supporting high-quality decision making and enabling care that aligns with their own goals and preferences.”
“This is the first generation of LGBT individuals who are out and through this study we hope to learn more about their knowledge and engagement with surrogate decision making and more about the barriers encountered by their surrogates,” Dr. Torke said.
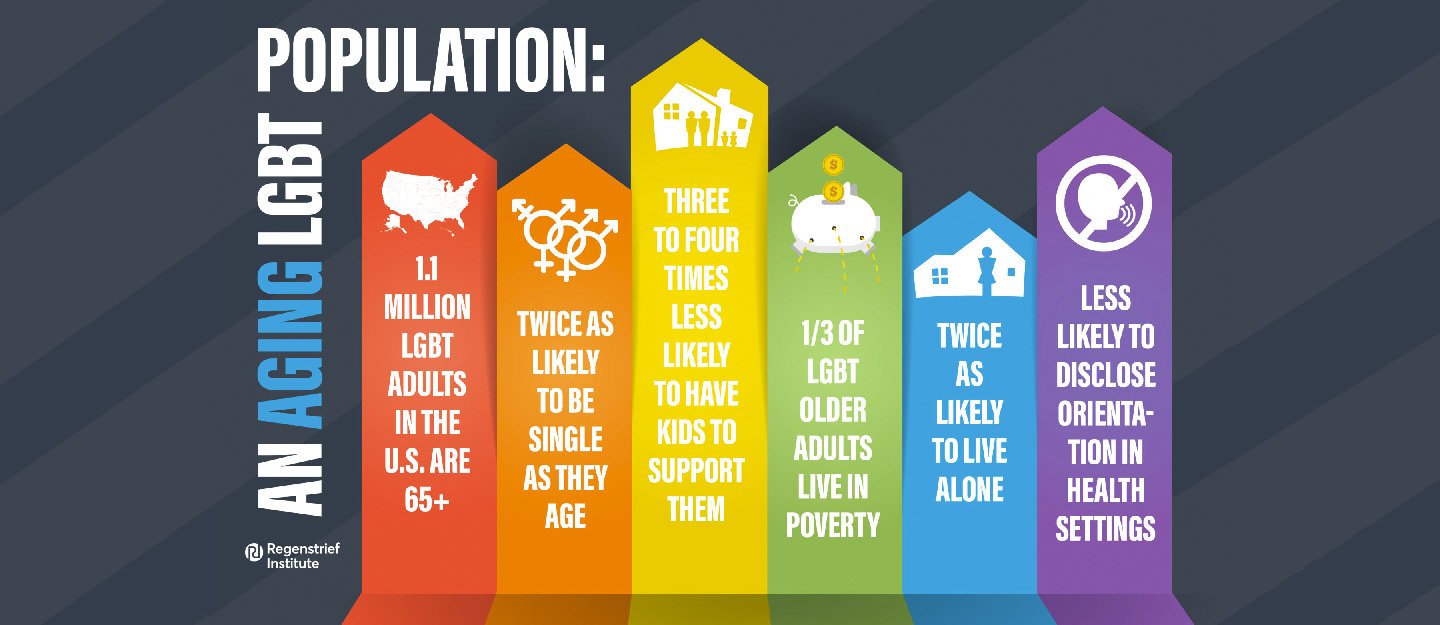
After encountering significant prejudice throughout their lives, LGBT individuals are known to confront even more prejudice as they grow older, according to Dr. Torke. Compared to heterosexual individuals, LGBT individuals are twice as likely to be single as they age, twice as likely to live alone, three to four times less likely to have children to support them, and Dr. Torke notes that because of these factors, LGBT individuals have increased challenges in advance care planning.
One third of LGBT older adults live in poverty. Currently, there are 1.1 million LGBT individuals in the United States who are 65 years of age and older. By 2030, it is estimated that this population will grow to 7 million. Because of social stigma, older LGBT individuals are known to refrain from disclosing their sexual orientation or going back in the closet as they age according to Dr. Torke. She notes that healthcare providers often operate without clear guidance on how to interact with LGBT individuals about care decisions and practices based on heteronormative assumptions.
The inclusion of same-sex partners in decision making and treatment planning has been shown repeatedly to be a priority for LGBT patients facing life-limiting illness.
In this newly funded study, Dr. Torke and colleagues from Regenstrief Institute, IU School of Medicine and Carey Candrian, Ph.D. from the University of Colorado Denver will explore the emotional, spiritual and religious experiences of both LGBT Alzheimer’s disease patients and their caregivers. Caregivers, who may be partners or spouses, children, other relatives or friends, will be interviewed and surveyed.
The researchers will explore the impact of communication quality on decision making quality and surrogate well-being, including post-traumatic stress. They will also examine religious and spiritual dimensions of surrogates and the extent to which they impact medical decision making as well as the actual care received by the LGBT individual with Alzheimer’s disease. The findings will inform the development of innovative aids to improve both the quality of medical care for incapacitated patients and the well-being of the decision makers.
This study of LGBT older adults with Alzheimer’s disease is supported by the National Institute on Aging of the National Institutes of Health under Award Number K24AG053794. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Dr. Torke is a co-author of the American Geriatrics Society Care of Lesbian, Gay, Bisexual, and Transgender Older Adults Position Statement issued in 2015.
About Regenstrief Institute
Founded in 1969 in Indianapolis, the Regenstrief Institute is a local, national and global leader dedicated to a world where better information empowers people to end disease and realize true health. The Regenstrief Institute and its researchers are responsible for a growing number of major healthcare innovations and studies. Examples range from the development of global health information technology standards that enable the use and interoperability of electronic health records to improving patient-physician communications, to creating models of care that inform practice and improve the lives of patients around the globe.
A key research partner to Indiana University, Regenstrief Institute is celebrating 50 years of healthcare innovation. Sam Regenstrief, a successful entrepreneur from Connersville, Indiana, founded the institute with the goal of making healthcare more efficient and accessible for everyone. His vision continues to guide the institute’s research mission.
About Alexia Torke, M.D., M.S.
In addition to her Regenstrief appointment, Alexia Torke, M.D., M.S., is an associate professor of medicine and associate chief of the Division of Internal Medicine and Geriatrics at Indiana University School of Medicine. She also directs the Daniel F. Evans Center for Spiritual and Religious Values in Healthcare at Indiana University Health.