A study conducted by Regenstrief Institute research scientists to examine the use, by older adults with Type 1 or Type 2 diabetes, of continuous use of glucose monitors and other wearable devices to assess and manage low blood sugar, has found that these tools pose both wearability and use problems for patients and their caregivers.
“This is a whole area of health technology that needs study. There’s hardware involved, which is the device itself. There’s software involved, which is reading, organizing, interpreting and communicating the data from the device. Knowing how the technology works in the real world and the impact of the technology on usability and ultimately on health outcomes is important,” said Michael Weiner, M.D., MPH, who led the study.
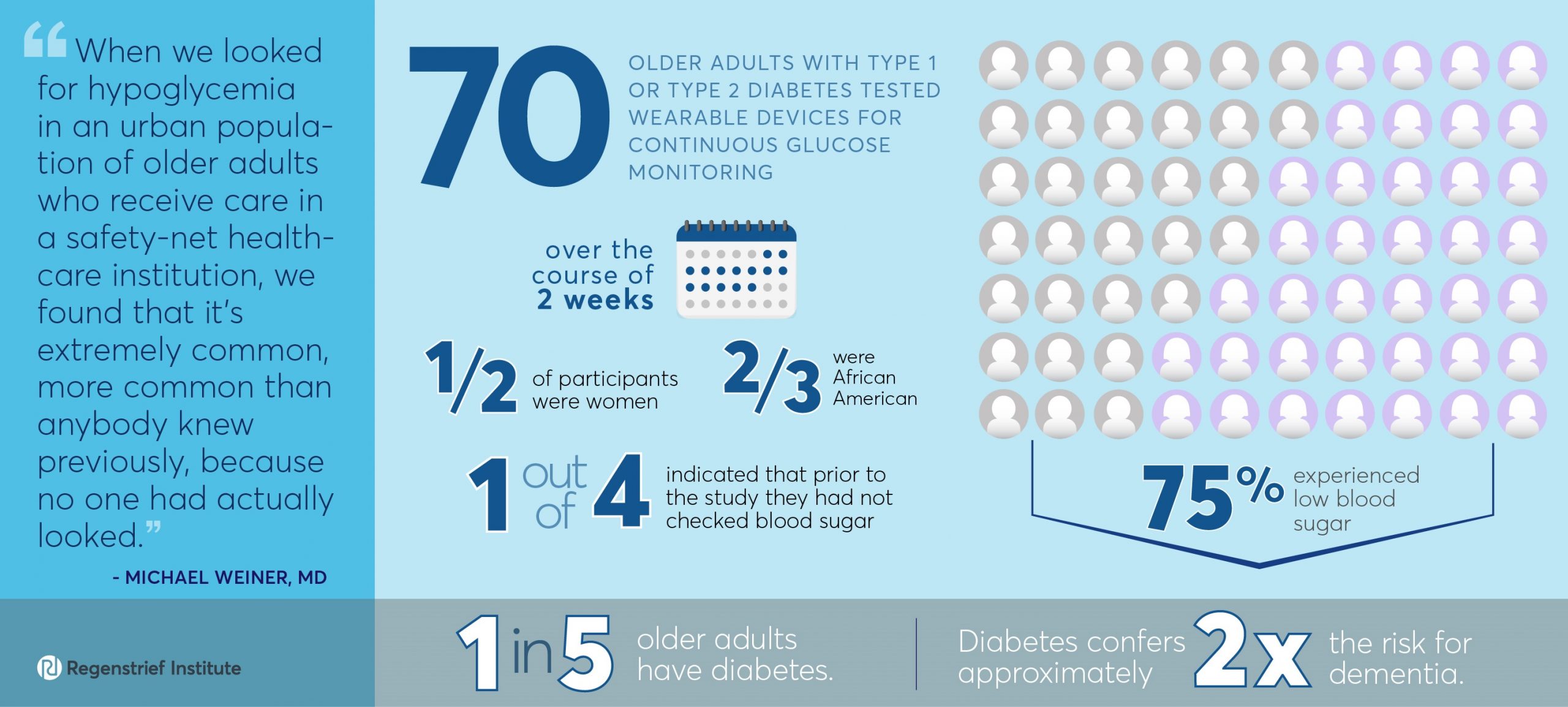
In an initial trial of continuous glucometer use, faulty device adhesive — a serious wearability challenge — and patient difficulty in interpreting graphs produced by the device, were noted. In a subsequent trial, 70 older adults with diabetes wore glucometers and activity monitors, and used smartphones and electronic medication bottles to track and manage blood sugar over a two-week period.
During these two weeks of monitoring, nearly three-quarters of the study participants experienced low blood sugar levels, often serious in magnitude. Among these 70 patients, two-thirds of whom were African American and more than half of whom were female, nearly one in four indicated that prior to the study, they had not checked blood sugar.
Diabetes is more common in the older population than the general population, with as many as one in five older adults having the disease. Hypoglycemia, also known as low blood sugar, is especially common in people with diabetes because of their medical condition as well as treatment that they receive for it. Both diabetes and hypoglycemia convey independent risks for dementia. Diabetes confers approximately a two-fold increased risk of dementia. The frequency of low blood sugar episodes among people with diabetes adds to that risk of dementia, independently.
Among the major findings of the study:
- Study participants found the glucose monitors and other wearable devices tricky to use, suggesting a need for device manufacturers to improve wearability and usability of the devices.
- Study participants were very interested in understanding their numbers (such as glucose levels) and the implications of these numbers.
- Nearly three-quarters of the study participants had low blood sugar (hypoglycemia), suggesting the need for monitoring devices to lead to more direct and effective management of blood sugar among older adults.
“When we looked for hypoglycemia in an urban population of older adults who receive care in a safety-net healthcare institution, we found that it’s extremely common, more common than anybody knew previously, because no one had actually looked,” said Dr. Weiner.
“That 73 percent of those in our study had low blood sugar is extremely concerning because hypoglycemia should always be addressed.
“Although a smartphone is very commonly used with continuous glucometers, we found that when we issued smartphones to study participants, they often didn’t carry the phones with them, contributing to the fact that, during the study, one-third of daytime phone prompts about medications, behaviors, and symptoms were ignored,” said Dr. Weiner. “And while I think there is a lot of future potential to use electronic medication bottles, we found study participants didn’t use them correctly or didn’t appropriately transfer their oral medications to the bottles.”
“Continuous Glucose Monitoring and Other Wearable Devices to Assess Hypoglycemia among Older Adult Outpatients with Diabetes Mellitus” is published in the peer-reviewed Applied Clinical Informatics. The study was supported by the Agency for Healthcare Research and Quality.
Authors are: Michael Weiner, M.D., MPH, Indiana University School of Medicine, Regenstrief Institute and Richard L. Roudebush VA Medical Center; Philip Adeoye, MSc, Regenstrief Institute; Margaret J. Boeh, Eskenazi Health; Kunal Bodke, Regenstrief Institute; Jessica Broughton, Eskenazi Health; Anietra R. Butler, Regenstrief Institute; Mackenzie L. Dafferner, Regenstrief Institute; Lindsay A. Dirlam, M.S., R.D., Eskenazi Health; Denisha Ferguson, Regenstrief Institute; Amanda L. Keegan, Regenstrief Institute; NiCole R. Keith, PhD, Regenstrief Institute and Indiana University; Joy L. Lee, PhD, M.S., Indiana University School of Medicine and Regenstrief Institute; Corrina B. McCorkle, Regenstrief Institute; Daniel G. Pino, M.D., Indiana University School of Medicine and Eskenazi Health; Mu Shan, Indiana University School of Medicine; Preethi Srinivas, Regenstrief Institute; Qing Tang, PhD, Indiana University School of Medicine; Evgenia Teal, Regenstrief Institute; Wanzhu Tu, PhD, Indiana University School of Medicine and Regenstrief Institute; April Savoy, PhD, Regenstrief Institute, Richard L. Roudebush VA Medical Center, Indiana University-Purdue University Indianapolis; Christopher M. Callahan, M.D., Indiana University School of Medicine, Regenstrief Institute and Eskenazi Health; Daniel O. Clark, PhD, Indiana University School of Medicine and Regenstrief Institute.
About Michael Weiner, M.D., MPH
In addition to his role as a research scientist at Regenstrief Institute, Michael Weiner, M.D., MPH is the principal investigator and director of the VA HSR&D Center for Health Information and Communication, Richard L. Roudebush VA Medical Center, and a professor of medicine at Indiana University School of Medicine.
About Regenstrief Institute
Founded in 1969 in Indianapolis, the Regenstrief Institute is a local, national and global leader dedicated to a world where better information empowers people to end disease and realize true health. A key research partner to Indiana University, Regenstrief and its research scientists are responsible for a growing number of major healthcare innovations and studies. Examples range from the development of global health information technology standards that enable the use and interoperability of electronic health records to improving patient-physician communications, to creating models of care that inform practice and improve the lives of patients around the globe.
Sam Regenstrief, a nationally successful entrepreneur from Connersville, Indiana, founded the institute with the goal of making healthcare more efficient and accessible for everyone. His vision continues to guide the institute’s research mission.
About IU School of Medicine
IU School of Medicine is the largest medical school in the U.S. and is annually ranked among the top medical schools in the nation by U.S. News & World Report. The school offers high-quality medical education, access to leading medical research and rich campus life in nine Indiana cities, including rural and urban locations consistently recognized for livability.